Author Bio: Dr. Ram Prakasha BPTh
Written by a Physiotherapy and Public Health professional with experience in neurological rehabilitation and health awareness. The content is intended for educational purposes only.
Alzheimer’s Disease is one of the most common and challenging neurological disorders affecting millions of people worldwide. As life expectancy increases, the prevalence of Alzheimer’s Disease is also rising steadily. Therefore, understanding this condition has become extremely important for patients, caregivers, and healthcare professionals. Moreover, early awareness can significantly improve quality of life. Alzheimer Disease is a progressive neurodegenerative disorder that mainly affects memory, thinking, behavior, and the ability to perform daily activities. Over time, it leads to a gradual decline in cognitive and physical functions. Consequently, individuals become increasingly dependent on others.
What Is Alzheimer’s Disease?
Alzheimer’s Disease is a type of dementia that causes irreversible damage to brain cells. Initially, it affects short-term memory; however, as the disease progresses, it impacts language, judgment, emotional control, and physical coordination. Eventually, even basic activities such as walking, eating, and speaking become difficult.
Furthermore, Alzheimer’s Disease develops slowly, often beginning years before noticeable symptoms appear. Because of this slow progression, early signs are frequently ignored or mistaken for normal aging.
Causes of Alzheimer’s Disease
Although the exact cause of Alzheimer’s Disease is still not fully understood, research suggests that multiple factors contribute to its development.
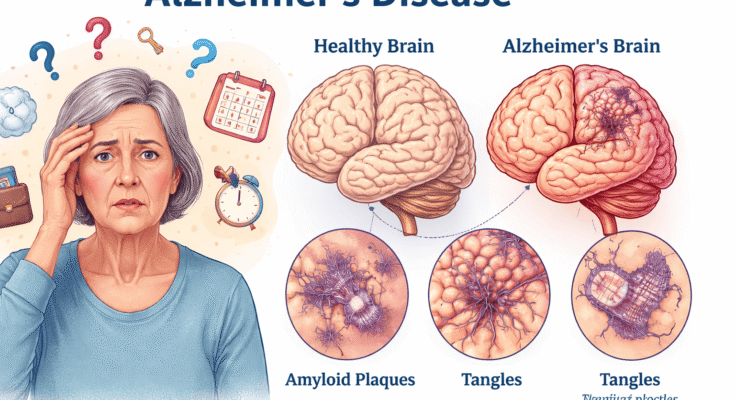
Firstly, abnormal protein accumulation in the brain plays a crucial role. Amyloid plaques and tau tangles interfere with communication between brain cells, leading to cell death.
Secondly, genetic factors can increase risk, especially in individuals with a family history of Alzheimer’s Disease.
Additionally, aging remains the greatest risk factor. Along with aging, conditions such as hypertension, diabetes, obesity, smoking, and a sedentary lifestyle further increase the likelihood of developing Alzheimer’s Disease.
Therefore, lifestyle modification is essential for prevention and delayed progression.
Early Signs and Symptoms
In the early stage, symptoms of Alzheimer’s Disease are mild and may go unnoticed. However, recognizing them early can help in timely intervention.
Common early symptoms include:
- Frequent memory loss
- Difficulty finding words
- Trouble concentrating
- Misplacing items regularly
- Mild confusion about time or place
As the disease progresses, symptoms become more severe. Consequently, individuals may experience personality changes, mood swings, anxiety, and depression.
Stages of Alzheimer’s Disease
Alzheimer’s Disease generally progresses through three main stages.
1. Mild (Early Stage)
At this stage, individuals remain mostly independent. However, subtle memory lapses and difficulty with complex tasks are evident.
2. Moderate (Middle Stage)
This is the longest stage. During this phase, memory loss worsens, confusion increases, and assistance with daily activities becomes necessary. Additionally, balance and coordination problems may start appearing.
3. Severe (Late Stage)
In the final stage, individuals lose the ability to communicate effectively and require full-time care. Mobility is severely reduced, and swallowing difficulties are common.
Diagnosis of Alzheimer’s Disease
Diagnosing Alzheimer’s Disease involves a combination of clinical assessment, cognitive testing, and imaging studies. Doctors often use memory tests, neurological examinations, MRI, and CT scans to rule out other conditions.
Although there is no single test that confirms Alzheimer’s Disease definitively, early diagnosis helps in planning treatment and supportive care.
Medical Treatment Options
Currently, there is no cure for Alzheimer’s Disease. However, medications can help manage symptoms and slow progression temporarily.
Commonly prescribed medications include:
- Cholinesterase inhibitors
- NMDA receptor antagonists
While these drugs improve cognitive symptoms to some extent, they do not stop disease progression. Therefore, non-pharmacological approaches such as physiotherapy play a vital role.
Role of Physiotherapy in Alzheimer’s Disease
Physiotherapy is an essential but often under-recognized component of Alzheimer’s Disease management. Although physiotherapy cannot reverse cognitive decline, it significantly improves mobility, balance, strength, and independence.
Moreover, physiotherapy helps reduce complications such as falls, muscle stiffness, joint contractures, and physical deconditioning.
Physiotherapy Goals in Alzheimer’s Disease
The primary goals of physiotherapy include:
- Maintaining functional mobility
- Improving balance and coordination
- Preventing falls
- Enhancing muscle strength
- Preserving independence for as long as possible
- Improving overall quality of life
Additionally, physiotherapy supports emotional well-being by encouraging movement and social interaction.
Physiotherapy Assessment
Before starting treatment, a detailed physiotherapy assessment is essential. This includes evaluation of:
- Muscle strength
- Joint range of motion
- Balance and gait
- Postural control
- Functional abilities
- Risk of falls
Based on this assessment, a personalized treatment plan is designed.
Physiotherapy Treatment Techniques
1. Exercise Therapy
Regular, structured exercise is the cornerstone of physiotherapy for Alzheimer’s Disease. Exercises improve circulation, muscle strength, and joint flexibility.
Examples include:
- Active range of motion exercises
- Strength training using body weight or resistance bands
- Stretching exercises to prevent stiffness
2. Balance and Gait Training
Since balance issues increase fall risk, physiotherapists focus on:
- Static and dynamic balance exercises
- Gait re-education
- Use of assistive devices when necessary
3. Functional Training
Functional exercises aim to improve daily activities such as:
- Sit-to-stand practice
- Bed mobility
- Walking short distances safely
4. Aerobic Conditioning
Low-intensity aerobic exercises like walking or stationary cycling improve cardiovascular health and brain oxygenation. Consequently, these activities may slow cognitive decline.
5. Postural Correction
Poor posture is common in later stages. Physiotherapy helps maintain spinal alignment and reduces pain and breathing difficulties.
Benefits of Physiotherapy in Alzheimer’s Disease
Physiotherapy offers multiple long-term benefits, including:
- Reduced fall risk
- Improved mobility and confidence
- Better sleep patterns
- Decreased caregiver burden
- Enhanced emotional well-being
Furthermore, regular physiotherapy sessions provide routine and structure, which is especially beneficial for individuals with Alzheimer.
Home-Based Physiotherapy and Caregiver Education
Home-based physiotherapy is highly effective because familiar surroundings reduce confusion and anxiety. Additionally, caregivers are educated on:
- Safe transfer techniques
- Proper positioning
- Simple daily exercises
- Fall prevention strategies
As a result, caregivers feel more confident and patients remain safer at home.
Lifestyle Modifications Along with Physiotherapy
Alongside physiotherapy, lifestyle changes play a critical role:
- Regular physical activity
- Healthy diet rich in antioxidants
- Adequate sleep
- Mental stimulation
- Social engagement
When combined, these approaches create a holistic management plan for Alzheimer’s Disease.
Prevention and Early Intervention
Although Alzheimer’s Disease cannot be completely prevented, early intervention can delay progression. Therefore, engaging in regular physical activity and physiotherapy from early stages is highly recommended.
Research shows that physically active individuals have a lower risk of developing severe cognitive impairment.
Frequently Asked Questions (FAQs)
1. Can physiotherapy cure Alzheimer’s?
No, physiotherapy cannot cure Alzheimer’s . However, it significantly improves physical function, mobility, and quality of life.
2. When should physiotherapy start in Alzheimer’s ?
Physiotherapy should start as early as possible, preferably in the mild stage, to maximize long-term benefits.
3. Is physiotherapy safe for geriatrics patients with Alzheimer’s ?
Yes, physiotherapy is safe when exercises are tailored to the individual’s abilities and supervised by a trained professional.
4. How often should physiotherapy sessions be conducted?
Ideally, sessions should be conducted 3–5 times per week, depending on the patient’s condition and tolerance.
5. Can physiotherapy reduce falls in Alzheimer’s ?
Yes, balance training and strength exercises significantly reduce fall risk.
6. Does exercise help brain function in Alzheimer’s Disease?
Regular physical activity improves blood flow to the brain, which may slow cognitive decline.
Conclusion
Alzheimer’s Disease is a life-altering condition that affects not only the individual but also families and caregivers. While there is no definitive cure, a comprehensive treatment approach can make a meaningful difference. Physiotherapy, when integrated with medical care and lifestyle modification, plays a powerful role in maintaining mobility, independence, and dignity.
Therefore, early diagnosis, consistent physiotherapy, and caregiver education together form the foundation of effective Alzheimer’s management. Ultimately, the goal is not just longer life, but a better quality of life.